What current research is being done for Frontotemporal dementia?
In the second of our blog series looking at less common types of dementia, we take a look at what research is ongoing into frontotemporal dementia.
In part one of this blog series we looked at some of the current research into vascular dementia. Now we'll be doing the same for frontotemporal dementia, formerly known as Pick's disease.
Let's start by learning a little more about the condition itself.
What is frontotemporal dementia?
Frontotemporal dementia gets its name because it affects the frontal and temporal lobes of the brain.
These parts of the brain are responsible for aspects such as behaviour, planning, understanding words and recognising faces. This means that people affected by frontotemporal dementia often have symptoms related to these aspects, for example changes in behaviour.
Different types of frontotemporal dementia include behavioural variant FTD and primary progressive aphasia. There are currently no treatments that can stop or slow down any form of frontotemporal dementia.
Frontotemporal dementia is relatively rare, but is a significant cause of dementia in younger people. Many people will develop the condition in their 40s and 50s, sometimes even in their 30s.
Current research into frontotemporal dementia
Development of frontotemporal dementia is linked to toxic clumps of proteins that are damaging to brain cells. Two proteins of particular interest to researchers are called tau and TDP-43.
As some (but not all) cases can run in families, there is also a great deal of research going into understanding the genetics of the condition. The genes that have been most strongly linked to frontotemporal dementia are called MAPT, GRN and C9orf72.
Many of Alzheimer’s Society’s researchers are working towards understanding frontotemporal dementia at the genetic and molecular level. For example, Dr Kurt de Vos at the University of Sheffield and Drs Ryan West and David Hicks at the University of Manchester are all working with cells in the lab or with fruit flies (which surprisingly give a really good insight into how genes work!) to uncover important information about how these genes and proteins influence the development of frontotemporal dementia.
Better understanding of the genetic changes and the effects these changes have on brain cells will help researchers to identify mechanisms and targets that could be suitable for the development of treatments.
Spotting frontotemporal dementia early
The only way to develop much-needed treatments for people with frontotemporal dementia is to enrol appropriate people in clinical trials that are testing potential therapies.
Researchers need to identify people who are affected by the condition as soon as possible to give the best chance of the potential treatment being successful and to give the maximum amount of benefit to the person affected.
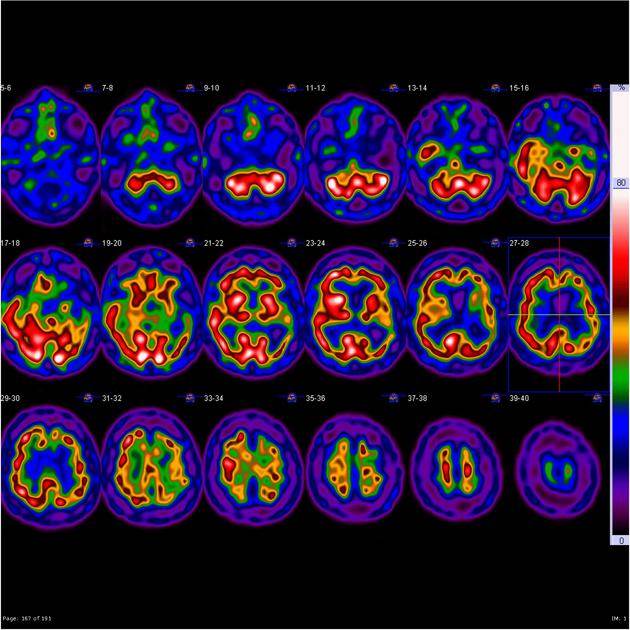
Professor Jason Warren and Dr Jon Rohrer at UCL have been developing a large programme of work to better understand frontotemporal dementia. This includes a project run by Professor Warren and funded by Alzheimer’s Society that uses brain scans to better identify frontotemporal dementia. These scans can tell us a lot about a person’s brain health, including whether their brain is shrinking or if there are any signs of damage.
Professor Warren and his team can link changes seen on brain scans with other symptoms of the condition to understand what is happening in people who are affected. This in turn will help diagnosis and early detection of frontotemporal dementia, allowing people to be enrolled in trials sooner.
Dr Rohrer's team are working on developing new memory and thinking tests, brain imaging and biological signals that will be used in drug trials. These tests will tell researchers and doctors when to start any treatment and whether those treatments are working. Dr Rohrer’s PhD student Katrina Dick, who is funded by Alzheimer’s Society, is developing a computer-based test that can help to identify subtle changes in thinking in people at risk of developing the genetic version of the condition. Katrina also co-ordinates the international Genetic FTD Initiative (GENFI).
Taking part in research studies
Dr Charles Marshall works as part of the UCL team, who are looking for people to take part in their studies. He explains:
'The team at UCL are working across lots of specialities to understand frontotemporal dementia better and to improve the chances of finding a treatment.
'We are looking for people with behavioural frontotemporal dementia or primary progressive aphasia (or those who know that one of these conditions runs in their family) to come for annual research visits, usually for two days. During this time they have scans, blood tests, detailed psychological testing and are given the option of having a lumbar puncture (spinal tap).
'We may also ask participants whether they would also like to take part in experiments designed to find out more about what is happening in the brain in frontotemporal dementia, and how particular symptoms arise. These can be fun, and usually involve watching videos or listening to music and other sounds on a computer, sometimes whilst in the MRI scanner.
'All this information allows us to find better ways to understand symptoms, diagnose and monitor frontotemporal dementia, including finding ways to measure whether treatments are working so that we can start planning trials of new medications.’
Would you like to take part in research?
If you have frontotemporal dementia or have a family history of frontotemporal dementia and are interested in studies, please email the UCL team or sign up to Join Dementia Research.


Carrianne Recla
saysRobert Gill
saysMy brother who is 71 was recently diagnozed with Frontal Lobe Dementia. My question, are there any studies where treatments are being given to see if FLD progress can be arrested?
Hi Robert,
Sorry to hear about your brother’s diagnosis.
For an overview of frontotemporal dementia (which is another word for frontal lobe dementia), our webpages can be a helpful place to start: https://www.alzheimers.org.uk/about-dementia/types-dementia/frontotempo…
In terms of studies and treatments, frontotemporal dementia is a very complex disease which can be caused by the build of different proteins in the brain. Therefore, lots of research is needed to understand the disease as well as find drugs to stop disease progression by trying to remove some of these proteins that build up.
Other studies look at treating the symptoms of frontotemporal dementia with some successful early trials for drugs and treatments. These have shown some drugs and treatments to be safe and effective in small groups of people, but more research is needed. There are now over 100 ongoing trials to further test these treatments as well as others. If you are interested in more detail about these, you could look at the clinical trials website to see a database of current and finished trials https://clinicaltrials.gov/ct2/results?cond=Frontotemporal+Dementia y=&dist=
If you are interested in being involved in research there is also Join Dementia Research, a service which can connect you with studies on dementia that you can volunteer for: https://www.joindementiaresearch.nihr.ac.uk/
If you or your brother need any dementia support, please call our Dementia Connect support line on 0333 150 3456. You can find more details about the support line (including opening hours) here: https://www.alzheimers.org.uk/dementia-connect-support-line
I hope this helps, Robert.
Alzheimer’s Society website team
Ms burns
saysPlease help, I’ve had two scans , first one said moderate frontal and mild temporal hypoperfusions in 2017 i
In 2019 or says persistent bilateral frontal hypoperfusions , I can’t get answers from anywhere . I’m so concerned
Hello Ms Burns,
We're very sorry to hear this - we can understand your concerns and frustration with lack of answers. Please arrange a consultation with your GP or medical consultant to discuss the results of your scans. They will be in the best position to help with this.
Our National Dementia Helpline advisers are available to provide support seven days a week on 0300 222 11 22 - here's more information about the Helpline: https://www.alzheimers.org.uk/get-support/national-dementia-helpline
Wishing you all the best
-
Alzheimer's Society blog team
Althea
saysI don't think frontotemporal dementia is "relatively rare" at all. I believe the disorder is under-recognized because it hides itself so very well.
It is frequently dismissed as marital breakdown or "midlife crisis," or misdiagnosed as depression, stress, anxiety, OCD, PTSD, late-onset ADHD, schizophrenia, bipolar disorder or alcoholism/drug-addiction because many of these these patients self medicate.
Mrs Ritchie
saysI LOOKED AFTER MY HUSBAND OVER LAST THIRTEEN YEARS VASCULAR DEMENTIA HE HAD TWO STROKES .AND FRONT LOBE IT WAS A
ONG JOURNEY HE HE WAS A STRONG MAN HE PASSED AWAY TWO WEEKS AGO I JUST CQME BACK FROM REST THE NURSING HOME NEGLECTED HIM SO NOW SOCIAL SERVICES SAFE GARDING AND DR OBSERVATION I HAVE SOLISITOR TO GET JUSTICE I M devestated
KS-Florida
saysMy father had FTD, unfortunately he lost his battle in February 2016. We do know that he was tested and was told that he did have the hereditary gene present. This absolutely horrifies me as I am now in my 40’s and have suffered numerous concussions and have various other health concerns.